Some of you may already know from my Facebook page that I recently experienced a kidney stone. I am sharing a few more details about the experience here on the blog as dehydration is one of the challenges of having an ileostomy and is something that can contribute to stone formation.
On Sunday, November 3rd, the NOAA forecast called for gorgeous weather. Doug and I had planned to head to the local crag for some climbing. Instead I woke up at 4:30 a.m. with a strange pain in my groin area. Doug heard me stirring, but since the pain was pretty minor, I told him to go back to sleep while I got up to make myself some tea and take a warm shower. Perhaps that would help it go away. I figured maybe I had just pulled a deep muscle, as I had gone for a pretty hard run the evening prior.
When I was in the shower, the pain started to get worse and it was strange because it felt like I already had to urinate again even though I had just gone when I got up. Great, I thought. I bet I am dealing with a urinary tract infection. I noted in my head that if things didn’t get better, I would schedule an appointment to see the doctor when the weekend was over.
After I got out of the shower, I sat down to go to the bathroom and suddenly felt an extremely sharp pain explode in my left flank. I knew right away that I was probably dealing with a kidney stone. I had had one 14 years ago and the pain was reminiscent of that experience. I also knew that this would likely require a trip to the ER. I started to make my way around the house to gather my insurance card, clothes, spare ostomy supply kit and other things I might need. I got about two minutes into that endeavor before I was brought to my knees by an even more intense pain. I crawled up the stairs and yelled for Doug to wake up and help me.
Seasoned from the days when I would wake up screaming from Remicade-induced joint pain or the times when I needed to be taken to the hospital late at night for UC flares, Doug sprang out of bed and into action at top speed as if he had rehearsed it 100 times. He helped me get dressed and he held my hair back when I began to vomit from the pain. I am not sure how I managed to walk on two feet out to the car, but soon we were zooming down the road to the hospital. Curled up in the front seat, I tried to use the mindfullness meditation techniques I had learned after surgery, and I attempted to focus on each breath instead of the waves of pain and nausea I was experiencing. When we got to the ER, Doug ran in to get a wheelchair while I waited doubled-over next to the car. A nurse heading in to start her shift rushed over to help. Within minutes, I was lying in a bed hooked up to an IV with some much needed Dilaudid.
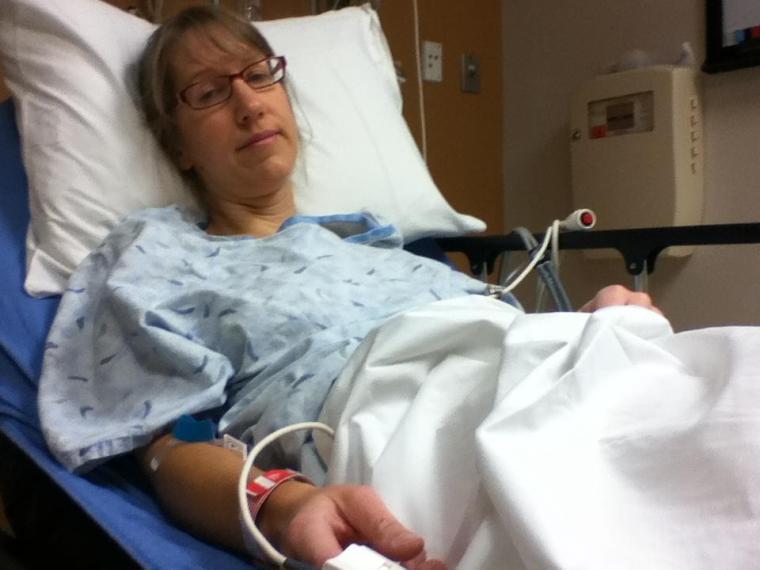
During my eight hours in the ER, the pain was so intense that I still hurt a lot even with the pain medication. The doctor decided to order a CT scan to see how big the stone was. Fortunately, it was 4mm: a size that I could likely pass on my own. However, I still couldn’t be released from the hospital until the stone moved to a place that was a bit less painful. I was sent home when I could finally hold down some Vicodin pills without throwing up. Before leaving, I was told the the CT scan also showed two more 4mm stones–one in each kidney. They couldn’t tell me if, or when, those would decide to make their way down the ureters.
When I got back to our house, Doug made me endless cups of herbal tea and I watched at least two tear-jerker dramas on Netflix which is one of my tried and true methods of feeling better. Every time I would get up to urinate, I would eagerly look in my strainer to see if the stone had passed. Finally, first thing the next morning, it popped out. I was so happy to see that little rock. It reminded me of a precious nugget in a gold pan! Once the stone passed, I had instant relief and was back to running and hiking within a couple of days.

My stone was sent to the lab to be analyzed later that week and I discovered it was the common calcium oxalate variety. I was given a sheet with recommendations for fluid intake and also a list of high-oxalate foods to avoid. Unfortunately, these foods are currently things that make up a larger portion of my diet: spinach, nuts, peanut butter, quinoa, legumes, oatmeal, berries, almond flour (which is a gluten-free baking staple) and chocolate. These are all things I eat a lot because I love them and I thought they were also good for me (well … except for the chocolate). Another thing I am supposed to avoid is salt. This is hard because when I exclude salt from my diet, I start to feel dizzy, weak and nauseated. Due to this and the fact that my blood pressure has gotten very low at times, my doctor recommended last year that I increase my sodium intake–especially when I am active. I feel that an appointment with a dietician may be in order to find out how to best manage having both an ileostomy and a predisposition to kidney stones.
While I wait for an upcoming follow-up appointment, I have been doing a little bit of research on kidney stones for a better understanding. I read that those with IBD and/or ileostomies can be prone to kidney stones due to the way these conditions affect urine volume, urine pH and calcium and oxalate excretion in the body. Interestingly, the calcium oxalate stone I had 14 years ago occurred at the same time I first developed ulcerative colitis symptoms. I am not sure if this is a mere coincidence, but definitely something to ponder.
The take-home message with all of this is that I need to drink a lot more water. I usually try to take in 3-4 liters in a normal day (more when I am doing something active). However, I also know that I have gotten a bit complacent with my hydration. Other than a few isolated times, I haven’t really felt dehydrated since surgery so I figured I was doing okay with my water intake. There were even a few times that I left my water behind on short runs because I thought I felt fine without it. I also got careless about drinking enough at work, oftentimes returning from leading a program to find the water bottle in my pack still full. I guess rather than giving me subtle signs that I needed more H2O, my body decided to give me a huge wake-up call in the form of a kidney stone. It is a lesson I won’t soon forget. In fact, I think it is time to go have a glass of water right now!


